Kas yra Merkelio ląstelių karcinoma?
Merkelio ląstelių karcinoma (MLK) yra reta ir agresyvi odos vėžio forma, kuri atsiranda iš Merkelio ląstelių, specializuotų neuroendokrininių ląstelių, esančių epidermio baziniame sluoksnyje. Šios ląstelės dalyvauja šviesos prisilietimo pojūtyje ir yra glaudžiai susijusios su nervų galūnėmis visame odoje. MLK klasifikuojama kaip neuroendokrininė karcinoma, todėl ji patenka į tą pačią plačią kategoriją kaip tam tikri plaučių ir virškinimo trakto vėžiai, kurie atsiranda iš hormonų gaminančių ląstelių. Nepaisant savo retumo, kasmet JAV diagnozuojama apie 3,000 naujų atvejų, MLK sulaukė vis didesnio dėmesio dėl savo agresyvaus elgesio ir atradimo, kad ji yra susijusi su specifiniu virusu.
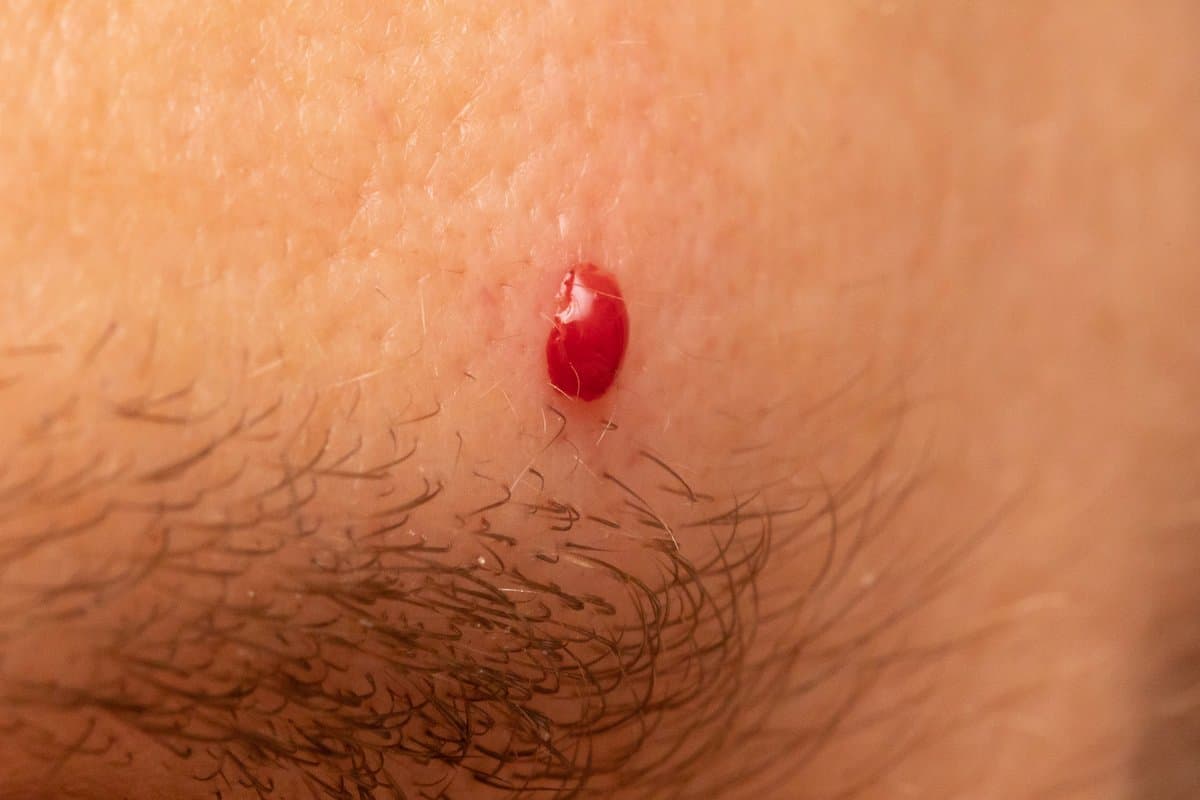
Retumas ir agresyvumas
Merkelio ląstelių karcinoma yra maždaug 30–40 kartų retesnė nei melanoma, tačiau ji turi žymiai didesnį mirtingumo rodiklį. Navikas turi stiprią tendenciją lokaliai atsinaujinti po pašalinimo, plisti į regioninius limfmazgius ir metastazuoti į tolimus organus, įskaitant kepenis, plaučius, smegenis ir kaulus. Apytiksliai trečdalis pacientų pirmo diagnozavimo metu turi limfmazgių pažeidimą, o bendras penkerių metų išgyvenamumo rodiklis visose stadijose yra apie 60 procentų.!! MLK agresyvumas iš dalies priklauso nuo jos greito augimo tempo ir gebėjimo plisti per limfinę ir kraujagyslių sistemą.
Kaip ji atrodo?
Merkelio ląstelių karcinoma dažniausiai pasireiškia kaip be skausmo, kieta, kupolo formos mazgelis odoje, kuris greitai auga per kelias savaites ar mėnesius. Spalva paprastai būna raudona, rožinė, violetinė arba mėlynai raudona, nors kartais ji gali pasirodyti odos spalvos. Paviršius paprastai yra lygus ir blizgus, o viršutinė oda gali turėti permatomą kokybę.
Klinikai kartais naudoja akronimą AEIOU, kad apibūdintų tipinius požymius: Asimptominis, Greitai plečiasi, Imuninė slopinimas, Vyresnis nei 50, ir UV spinduliams veikiama vieta. Dauguma navikų pasirodo ant galvos, kaklo ar galūnių, kurios yra sritys, turinčios didelį kumuliacinį saulės poveikį.

Rizikos veiksniai
Yra keletas gerai žinomų rizikos veiksnių, kurie prisideda prie Merkelio ląstelių karcinomos vystymosi. Lėtinis ir kumuliatyvus ultravioletinės spinduliuotės poveikis yra vienas iš svarbiausių, todėl MLK dažniausiai pasitaiko saulės veikiamoje odoje. Išsivysčiusio amžiaus faktorius taip pat yra svarbus, dauguma atvejų pasitaiko žmonėms, vyresniems nei 65 metų.
Imuninė slopinimas dramatiškai padidina riziką, o organų transplantacijos gavėjai susiduria su 10–15 kartų didesne tikimybe susirgti MLK. Merkelio ląstelių poliomavirusas (MCPyV) randamas integruotas į naviko ląsteles maždaug 80 procentų MLK atvejų.

Merkelio ląstelių karcinomos stadijos
Stadijos nustatymas yra kritinis žingsnis nustatant ligos išplitimą ir vadovaujant gydymo sprendimams dėl merkelių ląstelių karcinomos. Stadijų sistema atsižvelgia į pirminio naviko dydį, regioninių limfmazgių pažeidimą ir tolimų metastazių buvimą ar nebuvimą. I ir II stadijos liga yra apribota odai, o stadijų skirtumai priklauso nuo naviko dydžio.
III stadija rodo, kad liga išplito į regioninius limfmazgius. IV stadija atspindi tolimą metastazinę ligą. Sentinel limfmazgių biopsija rekomenduojama daugumai pacientų, sergančių MCC, nes net ir maži navikai turi didelę mikroskopinio limfmazgių pažeidimo riziką.
Gydymo metodai
Merkelio ląstelių karcinomos gydymas paprastai apima multimodalų požiūrį, derinant chirurgiją ir radioterapiją. Plati vietinė ekscizija su 1–2 centimetrų ribomis yra standartinis chirurginis gydymas pirminiam navikui, o sentinel limfmazgių biopsija paprastai atliekama tuo pačiu metu. Papildoma radioterapija pirminio naviko vietoje ir regioniniuose limfmazgiuose dažnai rekomenduojama, nes MCC yra labai jautri radiacijai. Pažengusiai ar metastazinei ligai gydyti imunoterapija su patikros inhibitoriais, tokiais kaip avelumabas arba pembrolizumabas, pastaraisiais metais pakeitė gydymo rezultatus, pasiekdama ilgalaikius atsakymus didelėje pacientų dalyje.

Prognozė ir išgyvenamumas
Merkelio ląstelių karcinomos prognozė labai skiriasi priklausomai nuo diagnozės stadijos. Pacientai, kuriems diagnozuota lokalizuota liga, apribota odai, ir kurie gauna tinkamą gydymą, turi penkerių metų išgyvenamumo rodiklius, svyruojančius nuo maždaug 50 iki 75 procentų. Kai yra pažeisti regioniniai limfmazgiai, penkerių metų išgyvenamumo rodiklis sumažėja iki maždaug 35–50 procentų.
Imunoterapijos įvedimas reikšmingai pagerino pacientų, sergančių pažengusia liga, rezultatus. Geresnę prognozę lemia mažesnis naviko dydis, limfmazgių pažeidimo nebuvimas, stipri imuninė sistema ir merkelių ląstelių poliomaviruso buvimas navike.

Stebėjimas ir ankstyvas nustatymas
Kadangi merkelių ląstelių karcinoma yra reta ir gali imituoti dažnesnių gerybinių odos būklių išvaizdą, sąmoningumas yra pirmas žingsnis ankstyvam nustatymui. Bet koks tvirtas, neskausmingas, greitai augantis mazgas ant saulės veikiamos odos, ypač asmeniui, vyresniam nei 50 metų arba turinčiam imuninį slopinimą, turėtų sukelti nedelsiant medicininę vertinimą.!! Po MCC gydymo intensyvus stebėjimas su reguliariais klinikiniais tyrimais ir vaizdavimo tyrimais yra standartinė praktika. Skinscanner gali būti naudingas palydovas reguliariam odos stebėjimui, leidžiantis dokumentuoti ir sekti bet kokius naujus ar besikeičiančius odos pažeidimus ir skatinti laiku konsultuotis su dermatologu.