Ano ang Molluscum Contagiosum?
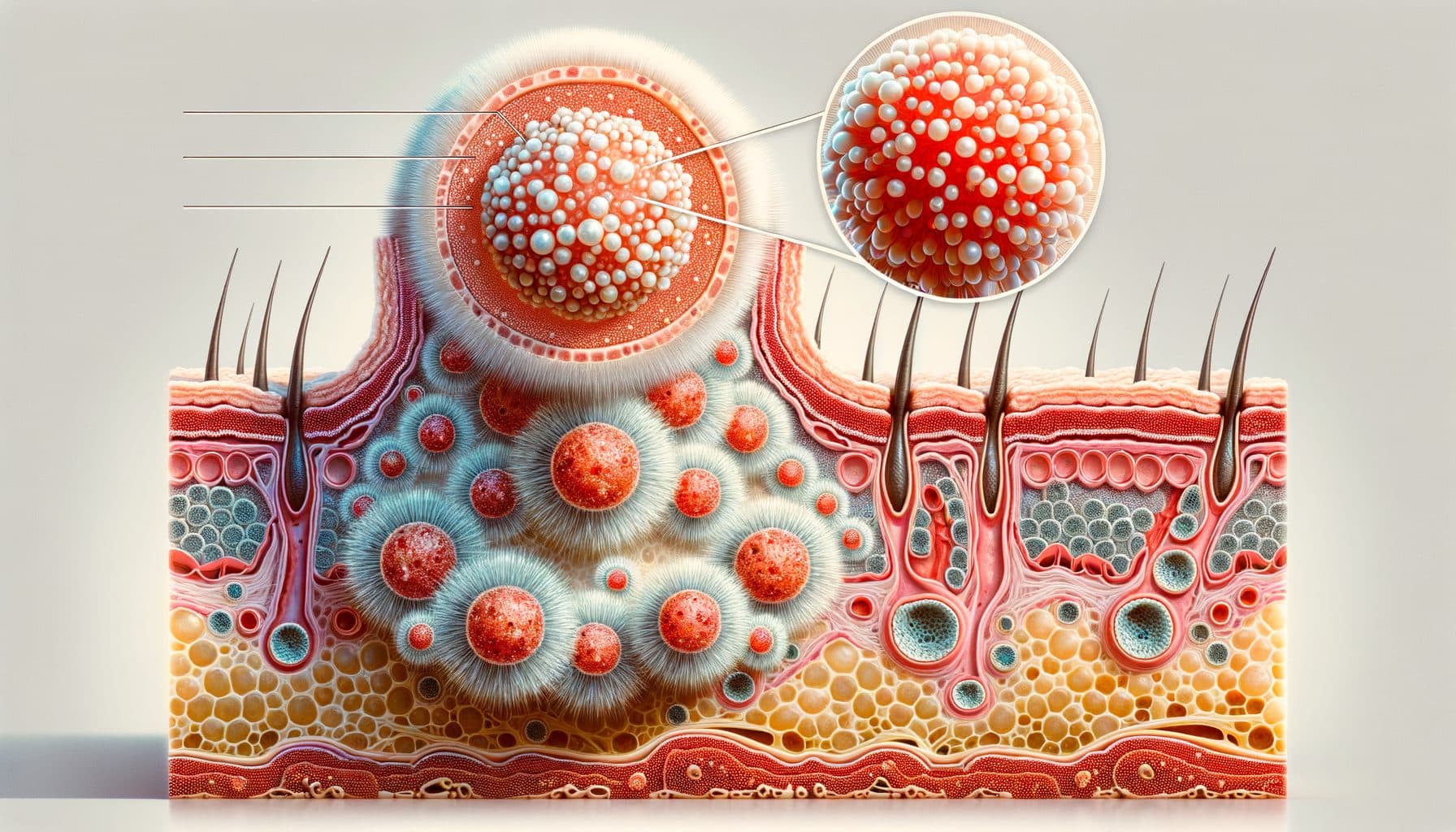
Ang molluscum contagiosum (water warts) ay mga benign na paglago sa balat na dulot ng molluscum contagiosum virus (MCV) mula sa pamilya ng poxvirus. Sa kabila ng pangalan, hindi sila tunay na kulugo (na dulot ng HPV). Karaniwang maliliit, 2–5 mm, perlas na mga nodule na may katangiang sentrong dimple (umbilication). Ang molluscum contagiosum ay pangunahing nakakaapekto sa mga bata sa pagitan ng 2 at 12 taong gulang ngunit maaaring mangyari sa anumang edad — sa mga matatanda, madalas itong naipapasa sa pamamagitan ng pakikipagtalik.
Paglipat at Mga Panganib na Salik
Ang virus ay naililipat sa pamamagitan ng direktang kontak sa balat o sa pamamagitan ng mga kontaminadong bagay (tuwalya, laruan, mga gamit sa swimming pool). Sa mga bata, ang impeksyon ay karaniwang nangyayari habang naglalaro, sa mga swimming pool, o kapag nagbabahagi ng mga bagay. Ang auto-inoculation — ang pagkalat sa ibang bahagi ng katawan sa pamamagitan ng pangangati — ay karaniwan.
Sa mga matatanda, ang sekswal na paglipat ay isang karaniwang ruta. Ang atopic dermatitis (eczema) ay isang mahalagang panganib na salik, dahil ang nasirang hadlang ng balat ay nagbibigay ng madaling access sa virus.!!
Mga Sintomas at Pagkilala
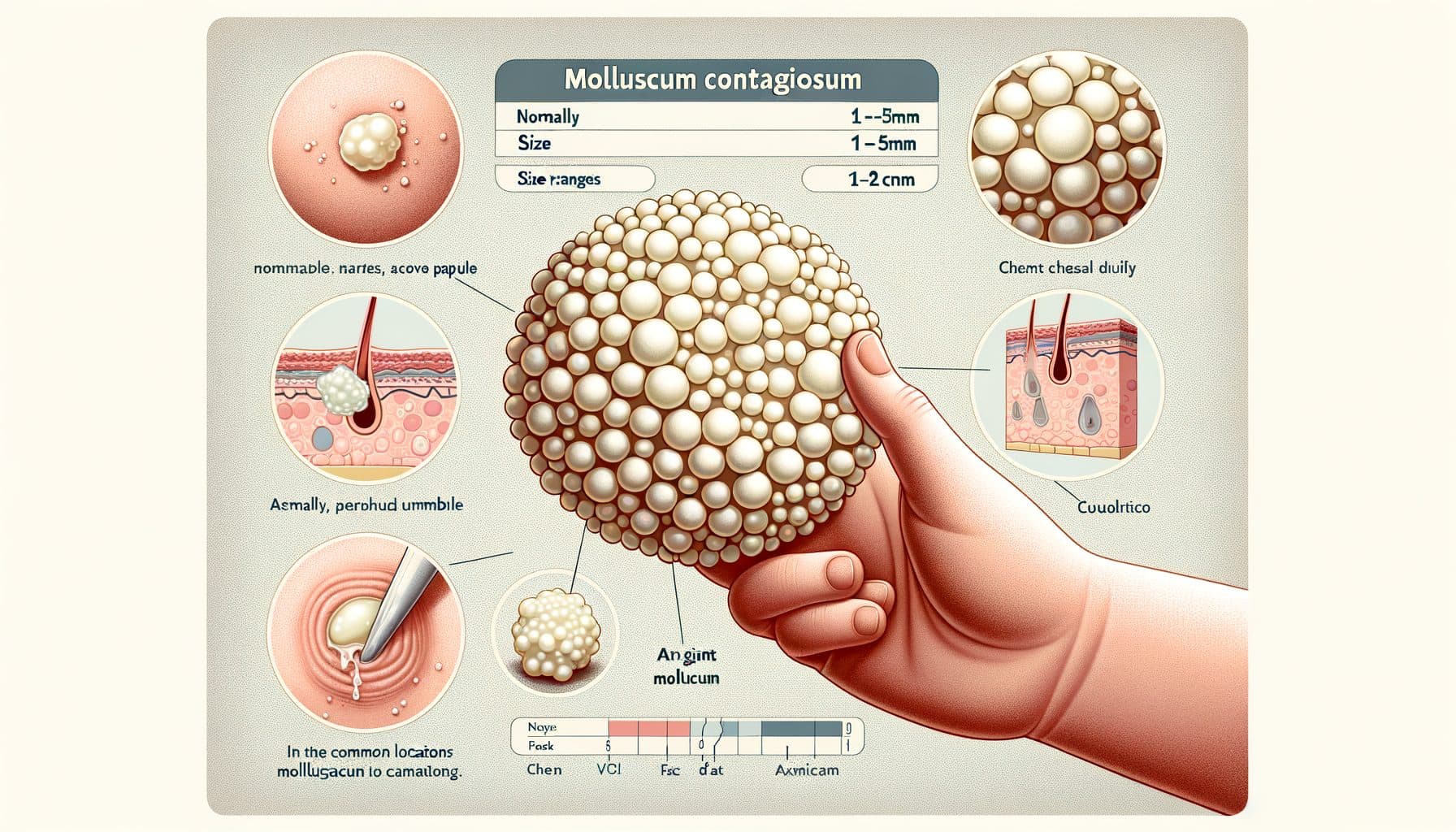
Ang molluscum contagiosum ay lumilitaw bilang bilog, makinis, perlas o kulay-balat na papules na may katangiang sentrong indentasyon (umbilication). Kapag pinisil, isang maputi, keso na masa ang lumalabas — ang tinatawag na molluscum body, na naglalaman ng napakaraming virus particles. Ang sukat ay mula 1–5 mm, bihirang umabot ng 1–2 cm (giant molluscum sa immunodeficiency).
Ang mga paboritong lugar sa mga bata ay ang katawan, mga dulo, kilikili, at mukha. Sa mga matatanda na may sekswal na paglipat, ang mga lesion ay matatagpuan sa genital at inguinal na rehiyon.
Diagnosis
Ang diagnosis ay klinikal, batay sa karaniwang hitsura — perlas na papules na may sentrong dimple. Ang dermoscopy ay nagpapakita ng isang karaniwang pattern na may sentrong butas o polychromatic amorphous structure na napapalibutan ng radial vessels (crown sign). Ang mga differential diagnoses ay kinabibilangan ng mga karaniwang warts, milia, mais, histoplasmosis, at sa mga pasyenteng may immunosuppression, cryptococcosis. Ang biopsy ay bihirang kinakailangan ngunit makakatulong sa mga atypical na presentasyon.
Mga Opsyon sa Paggamot
Dahil ang molluscum contagiosum ay self-limiting, ang mapanlikhang paghihintay ay katanggap-tanggap sa mga uncomplicated na kaso sa mga bata. Ang aktibong paggamot ay inirerekomenda para sa: pagkalat, pangangati, kosmetikong pagkabahala, sekswal na paglipat sa mga matatanda, o immunodeficiency. Ang mga opsyon ay kinabibilangan ng: curettage (pagsisipilyo ng mga nodule — mabilis ngunit maaaring mangailangan ng topical anesthesia sa mga bata), cryotherapy, potassium hydroxide solution (KOH 5–10% topical), cantharidin (extract ng blister beetle, available sa ilang bansa), at mga topical immunomodulators tulad ng imiquimod.
Kurso at Pag-iwas
Kung hindi ginamot, ang molluscum contagiosum ay nalulutas sa mga immunocompetent na indibidwal sa loob ng 6–18 buwan (minsan umabot ng 4 na taon). Bago mawala, ang mga lesion ay maaaring maging inflamed — isang senyales ng activated immune response (BOTE reaction: Beginning Of The End).!! Pag-iwas: iwasan ang direktang kontak sa balat sa mga lesion, huwag magbahagi ng mga tuwalya at gamit sa swimming, takpan ang mga lesion at huwag kamutin. Ang mga bata na may molluscum ay hindi dapat ibukod sa paglangoy, ngunit ang mga lesion ay dapat takpan.
Paano Makakatulong ang AI Skin Analysis
Madalas napapansin ng mga magulang ang maliliit na bukol sa balat ng kanilang anak at hindi sigurado kung ano ang mga ito — molluscum, warts, milia, o iba pa. Sinusuri ng Skinscanner ang hugis, katangian ng ibabaw, at ang nakababatid na gitnang dimple upang matulungan na matukoy kung ang mga bukol ay tumutugma sa molluscum contagiosum. Ang paunang pagsusuring ito ay makakapagpababa ng pagkabahala ng mga magulang at makakatulong sa iyo na magpasya kung ang mapanlikhang paghihintay ay angkop o kung dapat nang simulan ang paggamot.
Ang regular na pagkuha ng litrato ay mahalaga para sa pagsubaybay sa pagkalat ng mga lesion, pagdodokumento ng mga bago, at pagtukoy sa yugto ng pamamaga (reaksyong BOTE) na nagpapahiwatig na nililinis ng immune system ang virus. Para sa mga matatanda na may genital molluscum, makakatulong ang app sa paunang pagkilala bago humingi ng medikal na kumpirmasyon. Ang Skinscanner ay hindi pumapalit sa klinikal na diagnosis, ngunit nagbibigay ito ng madaling gabay para sa isang karaniwang kondisyon sa pagkabata na kadalasang nagdudulot ng higit na pag-aalala kaysa sa nararapat.


