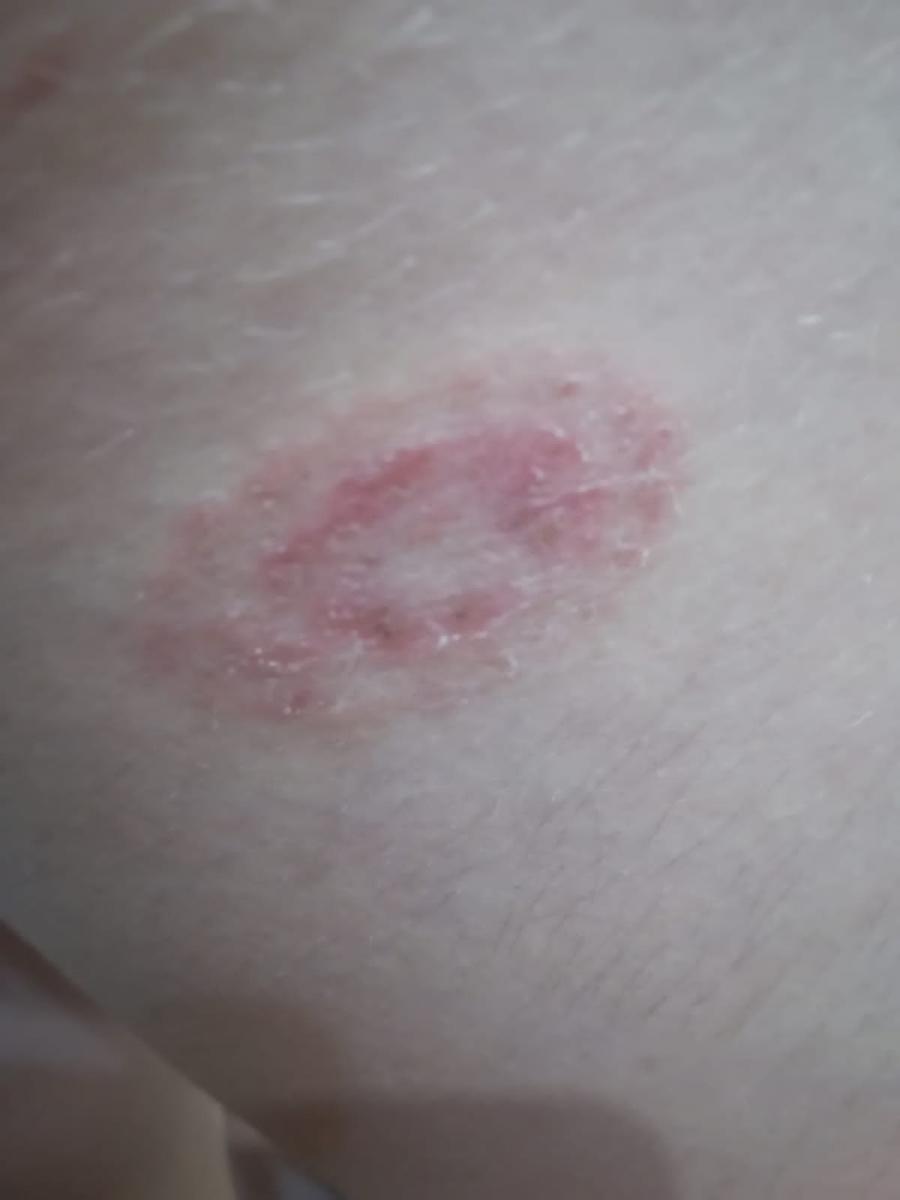
Les micosis cutànies són causades per diferents grups de fongs: dermatòfits (fongs semblants a floridures que s'alimenten de queratina a la pell, el cabell i les ungles), Candida (fongs semblants a llevats que normalment viuen al cos) i Malassezia (llevat que viu en àrees de pell greixosa). La infecció es desenvolupa o s'agreuja quan les condicions afavoreixen el creixement excessiu dels fongs, com calor, humitat, dany a la pell, roba ajustada o un sistema immunitari debilitat.
És més probable que desenvolupis micosi cutània si vius en un clima càlid i humit, sues molt, portes roba o sabates ajustades o no transpirables, comparteixes tovalloles o calçat, o tens condicions com diabetis, obesitat o un sistema immunitari debilitat. Els antibiòtics a llarg termini, esteroides o altres medicaments immunosupressors també augmenten el risc, especialment per a les infeccions per Candida.
La majoria de les micosis cutànies es tracten amb medicaments antifúngics tòpics (cremes, gels, esprais o xampús) aplicats una o dues vegades al dia durant diverses setmanes, i mantenint l'àrea neta, seca i ben ventilada. Les infeccions més extenses, recurrents o profundes, o les infeccions en persones amb immunitat dèbil, poden necessitar antifúngics orals amb recepta mèdica i supervisió mèdica.
Per prevenir les micosis cutànies, mantingues la pell neta i seca, especialment als plecs, entre els dits dels peus i a l'engonal; utilitza sabates i roba transpirables; i evita compartir tovalloles, sabates o navalles. Gestionar condicions com la diabetis, limitar els antibiòtics o esteroides innecessaris i tractar ràpidament petites taques fúngiques també pot reduir les recurrències.
Consulta a un metge si l'erupció s'està estenent ràpidament, és molt dolorosa o no millora després de 2-3 setmanes de tractament antifúngic adequat, o si tens diabetis, un sistema immunitari dèbil, o febre i et sents malament. Per a erupcions lleus i estables, pots utilitzar antifúngics sense recepta i monitoritzar els canvis amb la nostra anàlisi de pell per IA, però busca consell mèdic si no estàs segur del diagnòstic.
Normalment no perillós però pot estendre's o complicar-se; revisió mèdica necessària si és greu o persistent.