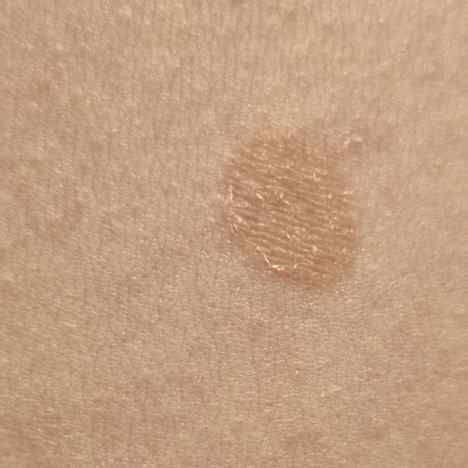
Årsaken til pityriasis versicolor er en overvekst og transformasjon av Malassezia-gjær som normalt lever på oljete hud. Varme, fuktighet, svette, oljete hud, hormonelle endringer, svekket immunforsvar og noen medisiner kan utløse dette skiftet og føre til synlige flekker.
Du er mer sannsynlig å få pityriasis versicolor hvis du bor i et varmt, fuktig klima, svetter mye, har oljete hud eller bruker stramme, ikke‑pustende klær. Hormonelle endringer, p-piller, systemiske steroider, svekket immunforsvar og underernæring øker også risikoen og gjør tilbakefall mer sannsynlig.
Mild pityriasis versicolor behandles vanligvis med soppdrepende sjampoer, løsninger eller kremer som ketokonazol, klotrimazol eller terbinafin, påført en eller to ganger daglig i 2–4 uker. Mer omfattende eller sta tilfeller kan trenge reseptbelagte tabletter som itrakonazol eller flukonazol, og selv etter at soppen er fjernet, kan fargeendringene ta uker til måneder å falme. Vår AI hudanalyse kan hjelpe deg med å spore hvor godt flekkene reagerer på behandling og om de begynner å komme tilbake.
For å forhindre pityriasis versicolor eller tilbakefall, hold huden så kjølig og tørr som mulig, bruk løse pustende klær og unngå svært oljete hudprodukter. Hos personer som har en tendens til å få hyppige tilbakefall, kan bruk av soppdrepende sjampo eller vask en gang i uken i varme, fuktige årstider redusere utbrudd, og vår AI hudanalyse kan hjelpe deg med å oppdage tidlige fargeendringer.
Du bør oppsøke lege eller hudlege hvis diagnosen er usikker, hvis reseptfrie soppdrepende behandlinger ikke hjelper etter 4–6 uker, eller hvis utslettet er omfattende, veldig kløende eller ser betent ut. En lege kan bekrefte diagnosen med en Wood-lampe eller KOH-test og avgjøre om du trenger reseptbelagte kremer eller tabletter.
Pityriasis versicolor er ikke en nødsituasjon og trenger vanligvis ikke akutt behandling, men du bør avtale en rutinemessig legetime eller hudlegebesøk hvis diagnosen er uklar, utslettet sprer seg, eller det ikke forbedres med standard soppdrepende behandling.