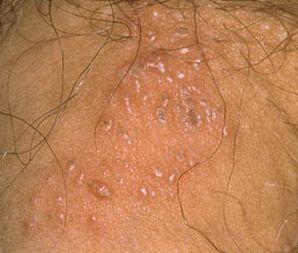
Genital herpes is caused by infection with herpes simplex virus, usually through sexual contact with an infected partner. HSV-1 or HSV-2 enters through tiny skin or mucosal breaks and then settles in nearby nerve cells, where it can reactivate later and cause new outbreaks.
You’re at higher risk of genital herpes if you have unprotected sex with multiple partners, have a partner with known herpes, or started sexual activity at a young age. Weakened immunity, other STIs, and frequent skin irritation in the genital area also increase the chance of infection and recurrences.
Genital herpes is treated with antiviral tablets such as acyclovir, valacyclovir, or famciclovir, which shorten outbreaks and reduce pain. Mild cases may only need local care like gentle washing, loose cotton underwear, warm baths, and painkillers, while frequent or severe outbreaks may require longer suppressive antiviral therapy prescribed by a doctor.
You can lower the risk of genital herpes by using condoms, limiting the number of sexual partners, and avoiding sex during outbreaks or when you feel warning signs like tingling or burning. Telling partners about your diagnosis, considering daily antiviral tablets if outbreaks are frequent, and managing triggers like stress and illness also help reduce recurrences and transmission.
See a dermatologist, venereologist, or sexual health doctor if you notice painful genital blisters, sores, or burning, especially after new sexual contact. Urgent assessment is needed if you have severe pain, trouble urinating, fever, are pregnant, or have a weakened immune system.
Genital herpes usually needs prompt but not emergency care, especially for a first episode or if symptoms are severe. Go to urgent or emergency care if you cannot urinate, have very strong pain, high fever, or are pregnant and think this is your first outbreak.