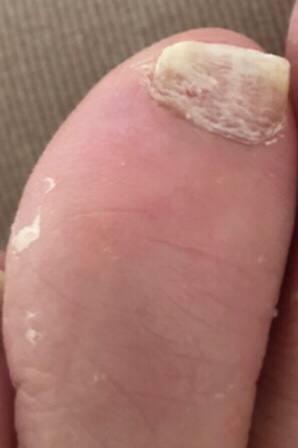
Onihomikozo povzročajo glivice, ki vdrejo v nohtno ploščo in nohtno posteljico, najpogosteje dermatofiti, kot je Trichophyton rubrum. Okužba se običajno začne, ko glivice vstopijo skozi majhne razpoke v nohtu ali okoliški koži, še posebej v toplih, vlažnih okoljih. Hoja bosa v skupnih tuših, nošenje tesnih čevljev ali atletsko stopalo povečuje možnost okužbe nohtov. Oslabljena imunost, diabetes in slaba prekrvavitev prav tako olajšajo, da se glivice naselijo.
Večje tveganje za onihomikozo imaš, če si starejši, imaš diabetes, slabo prekrvavitev ali oslabljen imunski sistem, ali če imaš pogosto potne noge ali atletsko stopalo. Tesni, neprepustni čevlji, hoja bosa v javnih tuših ali bazenih in poškodbe nohtov zaradi športa ali neustrezne obutve prav tako povečujejo tveganje. Ljudje, ki delajo v mokrih okoljih ali uporabljajo skupne garderobe, so bolj izpostavljeni. Družinska zgodovina glivic na nohtih in življenje z nekom, ki jih ima, lahko prav tako poveča tvoje možnosti.
Onihomikozo zdravimo z antimikotiki, bodisi peroralno, lokalno na nohtu ali oboje, odvisno od tega, koliko nohtov je prizadetih in kako resne so spremembe. Blage, površinske ali omejene okužbe nohtov se lahko odzovejo na medicinske lake za nohte ali raztopine, vendar debelejše ali obsežnejše okužbe običajno potrebujejo peroralne antimikotike več mesecev. Nohti rastejo počasi, zato je vidno izboljšanje potrebno nekaj časa, tudi po tem, ko je glivica nadzorovana. Redno spremljanje z našo AI analizo kože ti lahko pomaga spremljati napredek in se pogovoriti o rezultatih z zdravnikom.
Tveganje za glivice na nohtih lahko zmanjšaš tako, da ohranjaš stopala čista in suha, dnevno menjaš nogavice in izbiraš zračno obutev. Vedno nosi japonke ali sandale v javnih tuših, bazenih in garderobah ter se izogibaj deljenju ščipalcev za nohte, pilic ali čevljev. Zgodaj zdravi atletsko stopalo, da se ne razširi na nohte. Redno preverjanje nohtov, vključno z našo AI analizo kože, ti pomaga zgodaj zaznati spremembe in ukrepati, preden okužba postane resna.
Obišči zdravnika ali dermatologa, če opaziš trdovratno razbarvanje nohtov, zadebelitev, drobljenje ali ločitev od nohtne posteljice, še posebej, če je prizadetih več nohtov ali imaš diabetes ali slabo prekrvavitev. Zdravnik lahko potrdi diagnozo z laboratorijskimi testi in izbere najvarnejše in najučinkovitejše antimikotično zdravljenje zate. Uporabi našo AI analizo kože za spremljanje nohtov in prinesi slike ali poročila na obisk, da pomagaš usmerjati pogovor.
Onihomikoza običajno ni nujna in jo je mogoče oceniti na rutinskem obisku pri zdravniku ali dermatologu, vendar je ne smeš ignorirati, ker redko izgine sama od sebe. Poišči zgodnejšo oskrbo, če imaš diabetes, slabo prekrvavitev, znatno bolečino ali hitro poslabšanje sprememb na nohtih.