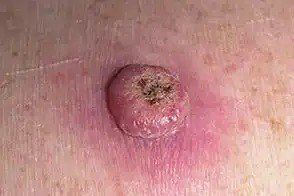
A causa exacta do queratoacantoma é descoñecida, pero a exposición prolongada ao sol, a radiación ionizante, a lesión cutánea crónica e o contacto con certos produtos químicos parecen aumentar o risco. É un tumor adquirido, non algo co que naces, e adoita aparecer máis tarde na vida adulta.
O queratoacantoma considérase unha condición opcional precancerosa: a maioría permanecen benignos, pero algúns poden transformarse en carcinoma de células escamosas, especialmente se son irritados ou queimados cronicamente. As persoas con queratoacantoma tamén teñen unha maior probabilidade de desenvolver outros cancros de pel preto ou noutros lugares da pel.
O tratamento principal para o queratoacantoma é a excisión cirúrxica cun pequeno marxe de pel sa, que elimina o tumor e permite un exame histolóxico preciso. O afeitado simple, a eliminación superficial ou métodos destrutivos como o láser ou a crioterapia non son ideais porque aumentan o risco de recorrencia e poden pasar por alto un cancro de pel subxacente.
Podes reducir o teu risco de queratoacantoma protexendo a túa pel da UV, evitando o trauma cutáneo crónico e minimizando a exposición á radiación ionizante e a produtos químicos agresivos. As auto-revisións regulares, a nosa análise de pel por IA e as visitas oportunas a un dermatólogo para calquera bulto novo ou cambiante son clave.
Se notas un bulto de rápido crecemento, en forma de cúpula, cunha crosta central ou un tapón semellante a un corno, especialmente en pel exposta ao sol, deberías ver a un dermatólogo ou oncólogo pronto. A nosa análise de pel por IA pode axudarche a monitorizar a lesión, pero só un médico cunha biopsia pode distinguir de forma fiable o queratoacantoma do cancro de pel.
Un bulto de rápido crecemento que podería ser queratoacantoma debería ser avaliado por un dermatólogo ou oncólogo nunhas poucas semanas, antes se é doloroso, sangra ou crece rapidamente. Non é unha emerxencia como unha infección grave, pero non debería ser ignorado ou observado durante meses sen revisión médica.