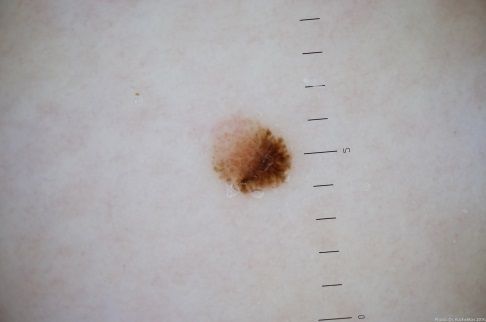
Düsplastilised neevused arenevad geneetilise eelsoodumuse ja keskkonnamõjude, peamiselt UV-kiirguse, koosmõjul. Hormonaalsed muutused, nahavigastused ja ioniseeriv kiirgus võivad samuti kaasa aidata, kuid tavaliselt pole ühel inimesel ühte selget põhjust.
Düsplastilised neevused kannavad suuremat riski muutuda melanoomiks kui tavalised sünnimärgid, eriti kui neid on palju, perekonnas on melanoomi ajalugu või on olnud tugev UV-kiirguse kokkupuude. Iga muutus suuruses, kujus, värvis, servas või uued sümptomid nagu sügelus, veritsus või koorik peaksid kiirelt arstlikku kontrolli saama.
Düsplastilise nevuse peamine ravi on kirurgiline eemaldamine koos väikese normaalse naha marginaaliga ja kohustusliku histoloogiaga. Hävitusmeetodeid nagu laser või külmutamine ei soovitata, sest need hävitavad koe ja muudavad melanoomi välistamise võimatuks.
Sa saad vähendada uute düsplastiliste neevuste ja melanoomi riski, piirates UV-kiirguse kokkupuudet, kasutades iga päev päikesekaitsekreemi, vältides solaariume ja ennetades korduvat traumat sünnimärkidele. Regulaarsed naha enesekontrollid, fotode jälgimine ja õigeaegsed visiidid dermatoloogi juurde on võtmetähtsusega.
Millal arsti juurde minna?
Sa peaksid nägema dermatoloogi või onkoloogi iga ebatüüpilise sünnimärgi puhul, eriti kui see muutub, erineb teistest sünnimärkidest või on kõrge riskiga inimesel või asukohas. Regulaarsed professionaalsed nahakontrollid, tavaliselt vähemalt kord aastas ja sagedamini, kui sul on palju düsplastilisi neevuseid, on tungivalt soovitatavad.
Kui ebatüüpiline sünnimärk muutub suuruses, kujus, värvis, servas või hakkab sügelema, veritsema või koorikuks muutuma, peaksid nägema dermatoloogi või onkoloogi järgmise 1–2 nädala jooksul. Stabiilsed ebatüüpilised sünnimärgid ilma muutusteta vajavad siiski regulaarseid planeeritud kontrolle, tavaliselt vähemalt kord aastas.