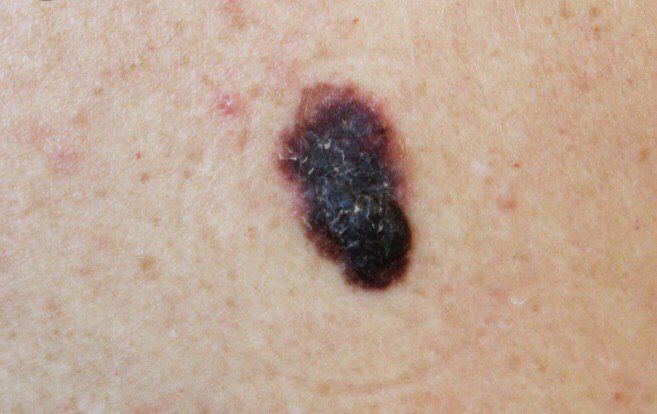
El melanoma es desenvolupa quan els melanòcits acumulen danys genètics i es tornen malignes, més sovint sota la influència de la radiació ultraviolada i susceptibilitat heretada. En moltes persones, no es pot identificar una causa clara única, però una barreja d'exposició a UV, tipus de pell i genètica hi juga un paper.
Els principals factors de risc per al melanoma són l'exposició intensa o repetida a UV, pell clara que es crema fàcilment, molts o lunars atípics, un historial personal o familiar de melanoma i edat avançada. La pell més fosca està una mica protegida, però els melanomes acral i subungueal encara ocorren i sovint es troben més tard.
El tractament principal per al melanoma és l'eliminació quirúrgica amb un marge de seguretat de pell normal al voltant del tumor. Si els ganglis limfàtics o òrgans distants estan implicats, el tractament també pot incloure cirurgia de ganglis limfàtics, immunoteràpia, teràpia dirigida, quimioteràpia i/o radiació, triat per un oncòleg segons l'etapa.
Pots reduir el teu risc de melanoma limitant l'exposició a UV, evitant llits de bronzejat, utilitzant protector solar d'ampli espectre i protegint la teva pell amb roba i ombra. Les auto-revisions regulars, la nostra anàlisi de pell amb IA per al seguiment de rutina i les visites oportunes al metge per a lunars canviants són igualment importants.
Qualsevol lunar o taca fosca que canviï de mida, forma, color o comenci a picar, sagnar o ulcerar ha de ser revisada urgentment per un dermatòleg o oncòleg. Utilitza la nostra anàlisi de pell amb IA per a revisions regulars, però no retardis una visita en persona si l'aplicació o la teva pròpia observació genera preocupació.
El melanoma és una emergència mèdica en el sentit que els retards poden ser potencialment mortals, per la qual cosa qualsevol lesió fortament sospitosa ha de ser avaluada per un dermatòleg o oncòleg en un termini de dies o, com a màxim, un parell de setmanes. Si un lunar està canviant ràpidament, sagnant o ulcerant, tracta'l com urgent i busca atenció en persona com més aviat millor.