Què És un Dermatofibroma?
Un dermatofibroma — també conegut com a histiocitoma fibros benign o histiocitoma cutis — és un creixement cutani comú i benigne compost per una barreja de fibroblasts, col·lagen i histiocits que forma un nòdul ferm i rodó dins de la dermis. Aquests creixements són dels lesions cutànies més freqüentment trobades en la pràctica dermatològica, representant aproximadament el tres per cent de totes les mostres cutànies enviades per a anàlisi patològica. Els dermatofibromes es presenten típicament com a nòduls ferms, rodons a ovalats, que mesuren entre cinc i deu mil·límetres de diàmetre, tot i que de vegades poden arribar a dos centímetres o més.
Se senten com un petit botó dur incrustat a la pell — notablement més ferm que el teixit circumdant. La pell que els cobreix pot ser del color de la pell, rosa, marró-rogenc o hiperpigmentada, i la superfície és generalment llisa, tot i que pot ser lleugerament escamosa o brillant. Els dermatofibromes es troben més comunament a les extremitats inferiors, particularment a les espinacs i cuixes, tot i que poden desenvolupar-se en qualsevol part del cos.
Són més prevalents en dones que en homes, amb la majoria apareixent en adults joves a mitjana edat entre els 20 i els 50 anys. Els creixements són típicament solitaris — tenir més d'un és comú, però múltiples dermatofibromes simultanis poden ocasionalment estar associats amb immunosupressió. Un cop formats, els dermatofibromes són generalment permanents i estables, sense créixer significativament ni resoldre's espontàniament.

Què Causa els Dermatofibromes?
La causa exacta dels dermatofibroms no està completament establerta, però es creu àmpliament que representen una proliferació fibrosa reactiva — essencialment un creixement excessiu de teixit similar a una cicatriu — desencadenat per una lesió cutània menor. Molts pacients poden recordar una picada d'insecte, una punxada d'espina, una esquitxada, un tall menor o fol·liculitis al lloc on es va desenvolupar posteriorment un dermatofibrom, recolzant la teoria de l'etiologia reactiva. La idea és que una ferida menor o una picada d'insecte desencadena una resposta inflamatòria localitzada, i durant el procés de curació, els fibroblasts i altres cèl·lules proliferan excessivament, produint un nòdul dens de teixit fibros que persisteix molt després que l'estímul original s'hagi resolt.
No obstant això, molts dermatofibroms apareixen sense trauma previ identificable, suggerint que hi ha factors addicionals en joc. Les influències hormonals poden contribuir — la major prevalença en dones i l'aparició o augment ocasional durant l'embaràs recolzen aquesta hipòtesi. El sistema immunitari també sembla jugar un paper, ja que les persones amb immunosupressió per infecció per VIH, trasplantament d'òrgans o medicaments immunosupressors tenen una major tendència a desenvolupar múltiples dermatofibroms.
Probablement existeix una predisposició genètica, ja que algunes persones desenvolupen nombrosos dermatofibroms mentre que altres no en desenvolupen cap malgrat una exposició similar a lesions cutànies menors. A nivell cel·lular, els dermatofibroms contenen una barreja de fibroblasts, miofibroblasts, histiocits i cèl·lules inflamatòries disposades en un patró característic en forma de llaç (en espiral) dins de la dermis. La lesió sovint s'estén al greix subcutani i atrapa els feixos de col·lagen circumdants a la seva perifèria, creant la fermesa característica d'aquests nòduls.

El Signe del Forat: La Pista Diagnòstica
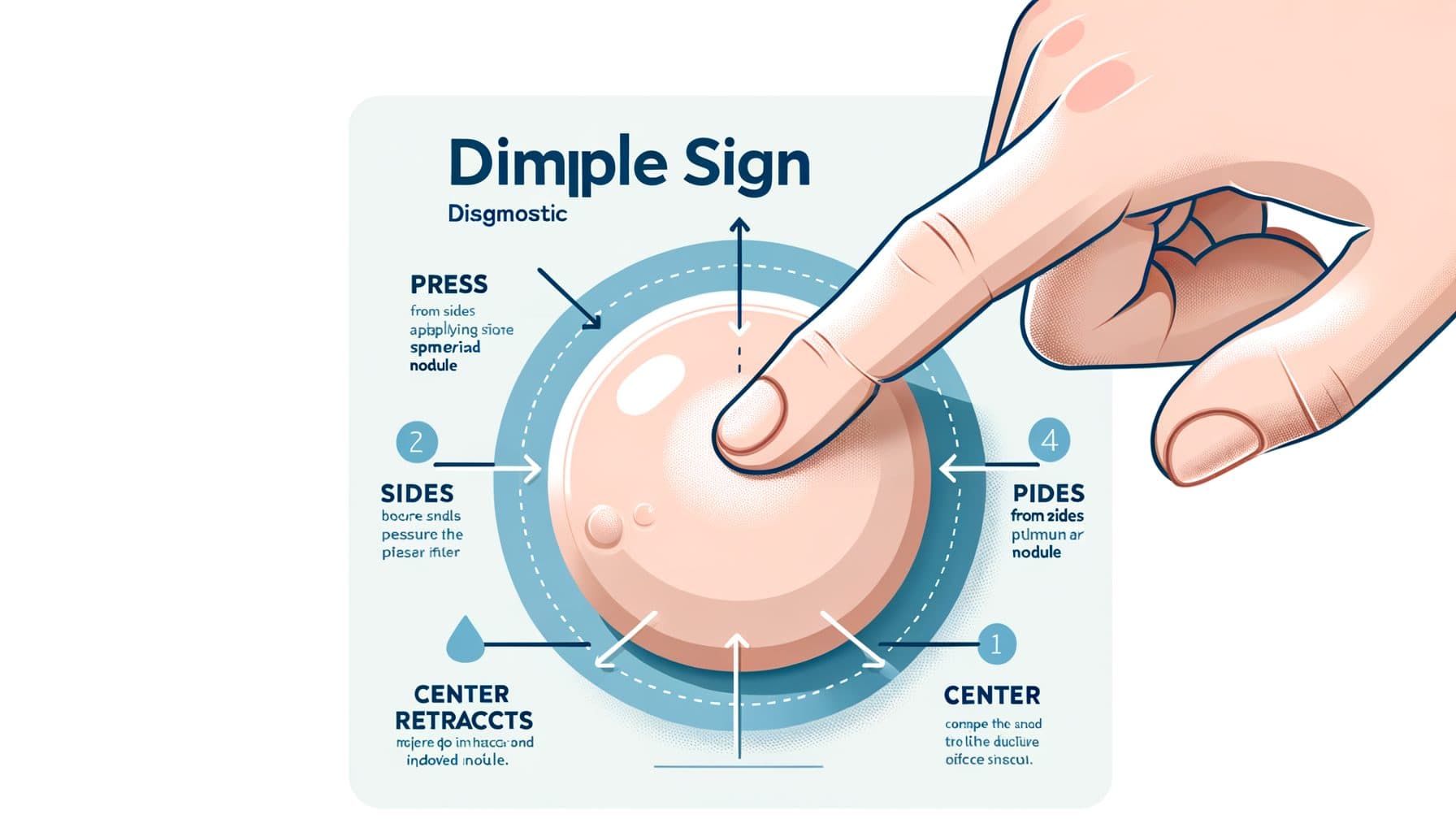
La característica clínica més distintiva d'un dermatofibrom és el signe del forat patognomònic — també anomenat signe de Fitzpatrick o signe de botó. Quan apretes la pell que cobreix un dermatofibrom entre el teu polze i l'índex, la lesió característicament s'enfonsa o es retreu cap a dins en lloc de protruir cap a fora com farien la majoria de les lesions cutànies elevades.!! Això ocorre perquè els dermatofibroms estan subjectes a la dermis circumdant per les seves extensions fibroses semblants a tentacles, i la compressió lateral provoca que la lesió sigui estirada cap avall al teixit subcutani.
El signe del forat és tan característic que per si sol pot establir el diagnòstic clínic en la majoria dels casos, tot i que no és completament específic — lesions malignes rares poden ocasionalment produir un signe similar. A més del signe del forat, diverses altres característiques ajuden a identificar els dermatofibroms. Són notablement ferms al tacte — més durs que la pell circumdant i la majoria de les altres lesions cutànies benignes.
La pell que els cobreix sovint mostra una decoloració marronosa que pot enfosquir-se amb l'exposició al sol. En dermatoscòpia, els dermatofibroms mostren un patró característic: una àrea central blanca semblant a una cicatriu envoltada per una delicada xarxa de pigment perifèrica, de vegades descrita com semblant a un paratge blanc envoltat per un anell marró de puntes. Aquest patró difereix de la xarxa de pigment que es veu en lesions melanocítiques i és reconeixible per a clínics formats. La fixació dels dermatofibroms dins de la dermis és una altra característica distintiva — es mouen amb la pell quan la llisques sobre el teixit subjacent però se senten ancorats dins de la pell mateixa, a diferència dels lipomes que són lliurement mòbils sota la superfície de la pell.
Dermatofibroma vs. Lesions Més Preocupants
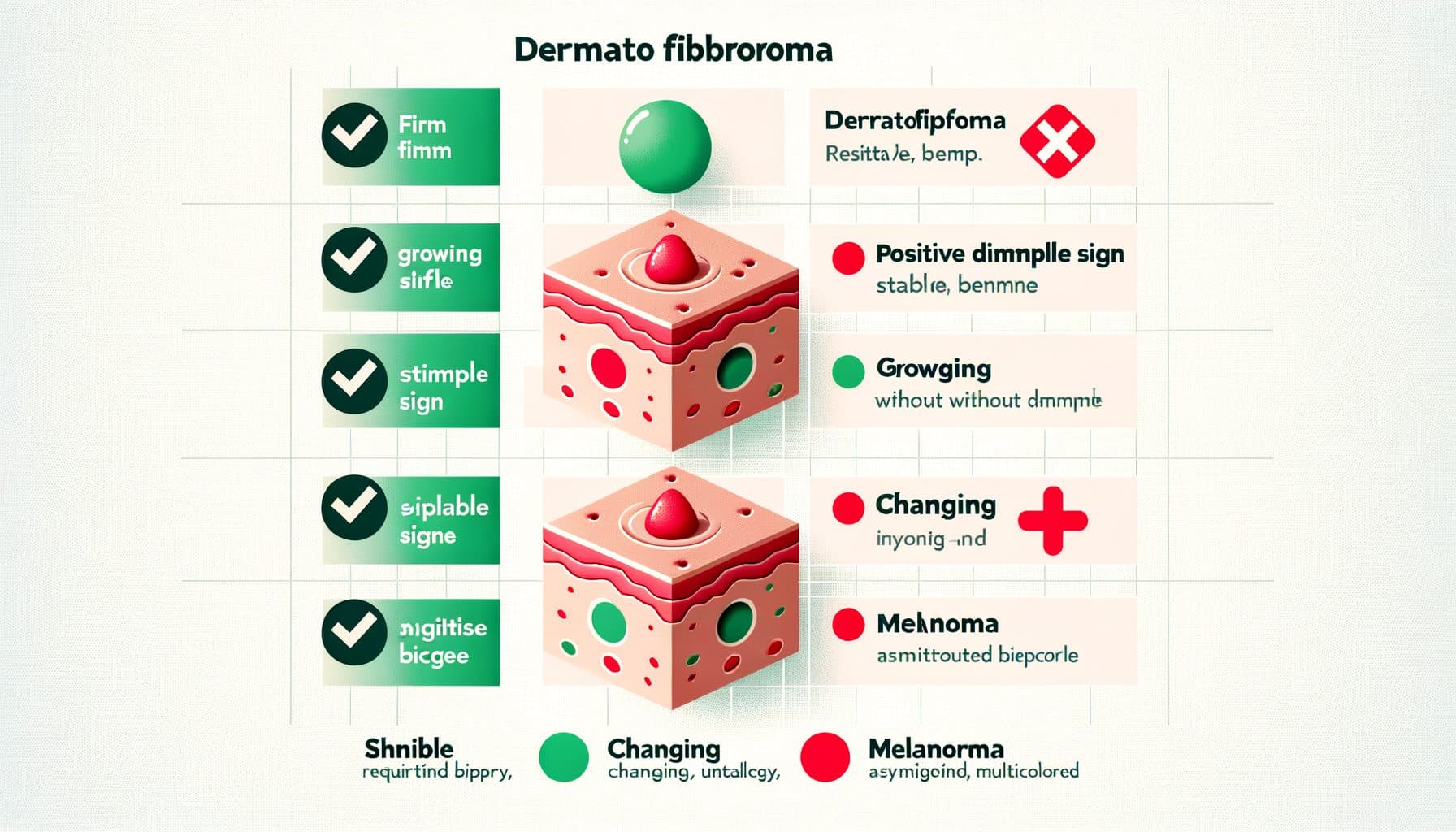
Encara que els dermatofibroms són benignes, diverses condicions més preocupants poden mimetitzar la seva aparença i s'han de distingir mitjançant una avaluació acurada. El dermatofibrosarcoma protuberans (DFSP) és un tumor de teixit tou rar, localment agressiu, que inicialment pot semblar un dermatofibrom. El DFSP tendeix a ser més gran, creix més ràpidament i sovint es localitza al tronc en lloc de les cames.
A diferència dels dermatofibroms, el DFSP s'estén profundament al teixit subcutani i a la fascia subjacent, té una taxa de recurrència més alta després de l'excisió i pot metastatitzar rarament. Qualsevol nòdul que creixi més de dos centímetres, s'ampliï progressivament o estigui fixat a estructures més profundes mereix una biòpsia per excloure el DFSP.!! El melanoma pot ocasionalment presentar-se com un nòdul firm, pigmentat que podria confondre's amb un dermatofibrom hiperpigmentat.
Les característiques que suggereixen melanoma inclouen asimetria, vores irregulars, variació de color incloent tons blau-negre o vermell, i un canvi recent en la mida o els símptomes. El signe del forat és típicament absent en el melanoma. El carcinoma basocel·lular, particularment els subtipus morfeiforme o nodular, pot presentar-se com un nòdul ferm de color de pell.
Busca una qualitat perlada translúcida, telangiectàsies a la superfície i absència del signe del forat. Un carcinoma de cèl·lules Merkel pot presentar-se com un nòdul ferm, de creixement ràpid, de color vermell a violet, sovint a la pell exposada al sol en pacients grans. Qualsevol nòdul cutani que estigui creixent ràpidament, canviant de caràcter, dolorós, sanguinolent o ulcerant hauria de ser biopsiat independentment de quant s'assembli a un dermatofibrom típic. El context és important — un nòdul ferm en un pacient immunosuprimido o algú amb un historial de càncer de pell mereix un llindar més baix per a la biòpsia.
Tractament: Quan i Com Eliminar Dermatofibroms
A causa que els dermatofibroms són benignes i no comporten cap risc de transformació maligna, el tractament no és mèdicament necessari. Molts pacients aprenen a viure amb els seus dermatofibroms un cop entenen la naturalesa benigna del creixement. No obstant això, l'eliminació pot ser desitjada per diverses raons: preocupacions estètiques, especialment per lesions en àrees visibles com les espinces o els braços; irritació recurrent per afaitar, fricció de la roba o trauma repetit; tendresa persistent o dolor (alguns dermatofibroms són incòmodes quan es pressionen); incertesa diagnòstica on es necessita una biòpsia per descartar una lesió més preocupant; o una ansietat significativa del pacient malgrat la tranquil·lització.
L'excisió quirúrgica completa és el tractament definitiu però ve amb una advertència important: a causa que els dermatofibroms s'estenen profundament a la dermis i de vegades al greix subcutani, l'excisió completa requereix tallar força profund, resultant en una cicatriu quirúrgica que pot ser més visible estèticament que la lesió original — particularment a les cames, on la cicatrització tendeix a ser més lenta i visible. Els pacients haurien de ser assessors sobre aquest intercanvi abans de procedir. L'excisió per afaitat (eliminació tangencial) elimina la porció visible del dermatofibrom a nivell de la superfície de la pell o just per sota, deixant una cicatriu més plana.
No obstant això, a causa que la porció més profunda roman, les taxes de recurrència són més altes — reportades en un 20% o més. La crioteràpia amb nitrogen líquid pot aplanar els dermatofibroms però rarament els elimina completament i pot deixar marques hipopigmentades. El tractament amb làser s'ha utilitzat amb èxit variable. Per a la majoria dels pacients, l'enfocament pragmàtic és l'observació amb tranquil·lització, reservant l'excisió per a lesions que són sintomàtiques, diagnòsticament incertes o que causen un estrès estètic significatiu.

Com l'Anàlisi de Pell AI Pot Ajudar
Descobrir un bony ferm a la teva pell comprensiblement genera preguntes i, de vegades, ansietat. És només un dermatofibrom inofensiu, o podria ser alguna cosa més seriosa? Skinscanner proporciona una anàlisi immediata impulsada per IA quan fotografies un nòdul cutani preocupant, avaluant característiques com el color, la forma, les característiques de la vora i la textura de la superfície per ajudar a determinar si la lesió és consistent amb un dermatofibrom benigne o presenta característiques que mereixen una avaluació professional.
La IA pot reconèixer patrons comuns associats amb els dermatofibroms — la decoloració marronosa, la forma rodona simètrica i la superfície llisa — i distingir-los de patrons més suggeridors de lesions preocupants com el dermatofibrosarcoma protuberans o el melanoma. Per a les persones amb múltiples dermatofibroms, Skinscanner ajuda a monitorar les lesions existents per a qualsevol canvi i identificar nous creixements que difereixin del patró establert. Encara que el signe del forat característic no es pot avaluar només a través de la fotografia, les característiques visuals capturades en una foto d'alta qualitat proporcionen informació diagnòstica valuosa.
Skinscanner és particularment útil com a eina de detecció de primera línia per a l'escenari comú de descobrir un nou bony ferm i voler orientació immediata sobre si és necessària una avaluació urgent. No substitueix l'examen clínic — qualsevol nòdul que estigui creixent, canviant, sintomàtic o preocupant malgrat la tranquil·lització de la IA hauria de ser avaluat per un dermatòleg que pugui realitzar palpació, dermatoscòpia i biòpsia si és necessari.


