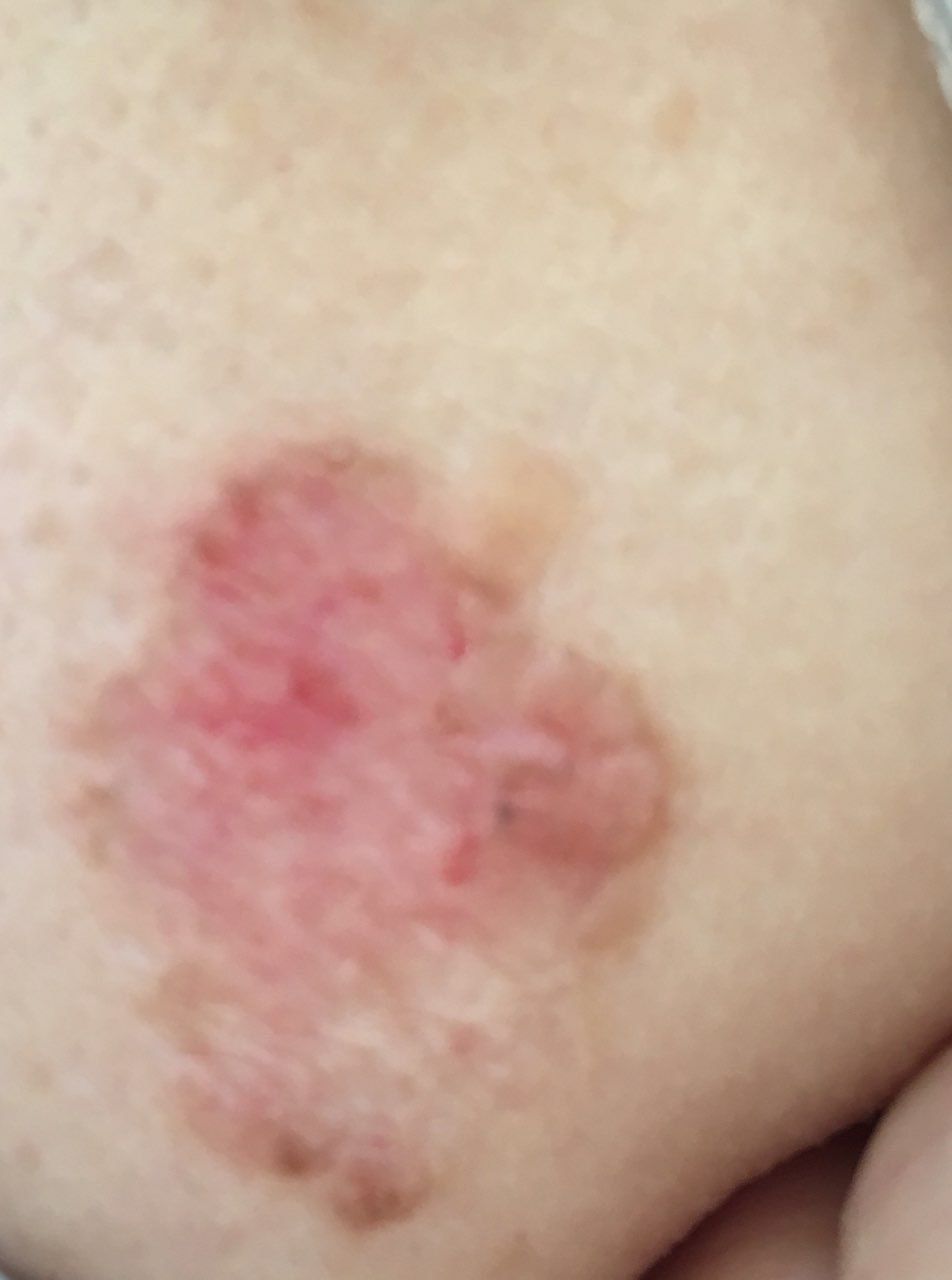
স্কোয়ামাস সেল কার্সিনোমার কোনো একক কারণ নেই, তবে দীর্ঘমেয়াদী UV এক্সপোজার, রেডিয়েশন, কিছু রাসায়নিক, দীর্ঘস্থায়ী ত্বকের ক্ষতি এবং কিছু বিরল ত্বকের রোগ ঝুঁকি বাড়ায়। কিছু ক্ষেত্রে, মানব প্যাপিলোমাভাইরাস (HPV) এবং দুর্বল ইমিউন সিস্টেমও ভূমিকা পালন করে।
চিকিৎসার পর SCC ফিরে আসতে পারে এবং কিছু ক্ষেত্রে এটি কাছাকাছি লিম্ফ নোড বা দূরবর্তী অঙ্গে ছড়িয়ে পড়তে পারে, বিশেষ করে যখন এটি বড়, গভীর বা দীর্ঘস্থায়ী হয়। একবার SCC হওয়া ব্যক্তিদের ভবিষ্যতে নতুন ত্বকের ক্যান্সার হওয়ার সম্ভাবনা বেশি এবং নিয়মিত ত্বক পরীক্ষা প্রয়োজন।
স্কোয়ামাস সেল কার্সিনোমার প্রধান চিকিৎসা হল টিউমারটি সম্পূর্ণরূপে অপসারণ করা এবং এর চারপাশে সুস্থ ত্বকের একটি প্রান্ত রাখা। আকার, গভীরতা এবং অবস্থানের উপর নির্ভর করে, ডাক্তাররা রেডিওথেরাপি, বিশেষায়িত সার্জারি (যেমন মোহস), বা উন্নত ক্ষেত্রে সিস্টেমিক চিকিৎসা যেমন ইমিউনোথেরাপি বা কেমোথেরাপি ব্যবহার করতে পারেন।