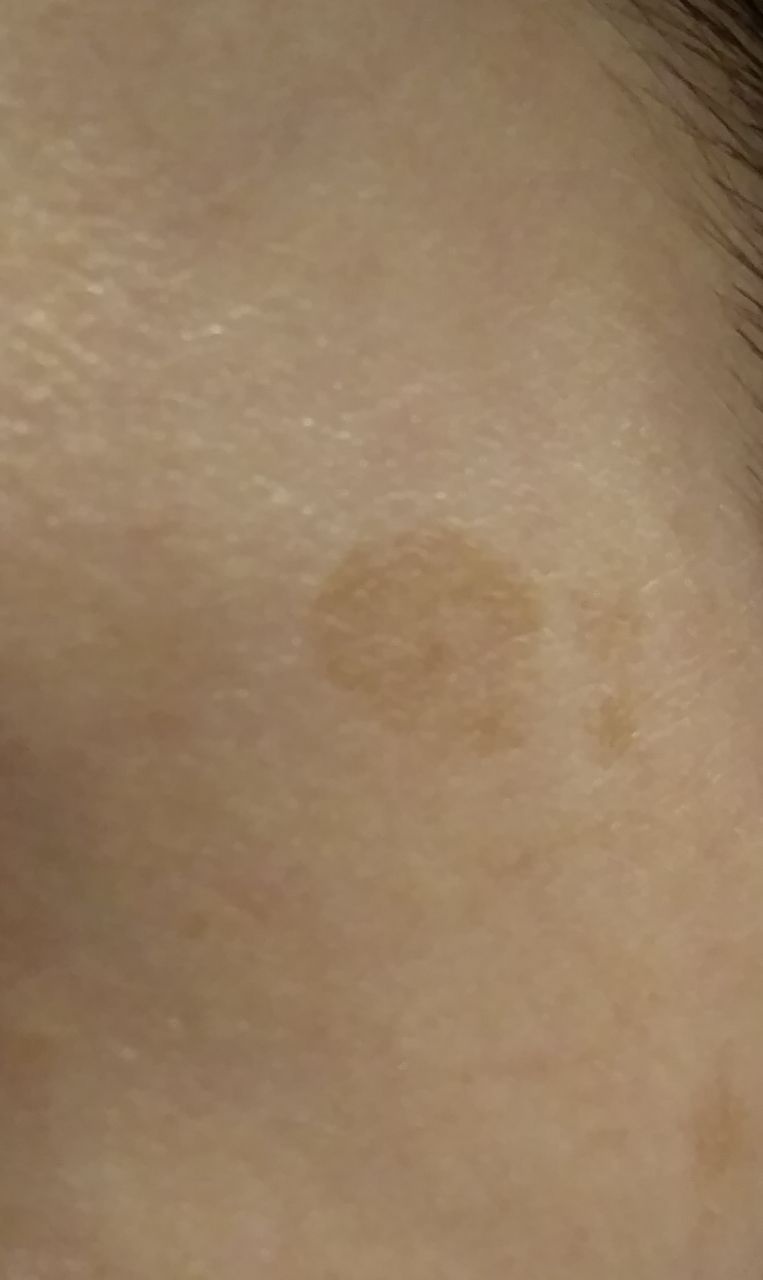
Lentigo se vyvíjí, když určité kožní buňky produkují extra melanin, obvykle po letech vystavení UV záření ze slunce nebo solárií. Věk, světlá pleť, hormony, genetika a někdy předchozí poškození kůže nebo radiace také hrají roli. U mladších lidí je lentigo méně časté a může být spojeno s hormonálními nebo metabolickými problémy. Často se spíše sčítá několik faktorů než jedna jediná příčina.
Jednoduché lentigo samo o sobě má velmi nízké riziko přeměny na melanom, podobně jako normální kůže. Hlavní riziko spočívá v tom, že se přehlédne časný melanom nebo lentigo maligna, které vypadají jako neškodná sluneční skvrna. Další vystavení UV záření, chronické podráždění a vyšší věk zvyšují celkové riziko rakoviny kůže. Pravidelné samokontroly, naše AI analýza kůže a periodické návštěvy u dermatologa pomáhají udržet toto riziko pod kontrolou.
Většina lentigů nepotřebuje léčbu, pokud se ti nelíbí, jak vypadají, nebo pokud je skvrna v oblasti s vysokým rizikem, která je neustále vystavena tření. Možnosti zahrnují chirurgické odstranění jednotlivých lézí a kosmetické metody, jako jsou lasery, chemické peelingy nebo světelné procedury pro více skvrn. Jakýkoli destruktivní zákrok by měl být proveden pouze po vyšetření dermatologem nebo onkologem, ideálně s dermatoskopií nebo biopsií, pokud je to nutné. Po odstranění by měla být oblast sledována na nové nebo recidivující pigmenty, pomocí fotografií nebo naší AI analýzy kůže.
Můžeš snížit šanci na nové lentigo a snížit riziko rakoviny omezením vystavení UV záření, vyhýbáním se soláriím a používáním denního širokospektrálního opalovacího krému. Noste klobouky a ochranné oblečení, vyhýbej se chronickému tření nebo podráždění stejných oblastí kůže. Dodržuj bezpečnostní pravidla, pokud pracuješ s radiací nebo chemikáliemi poškozujícími kůži. Pravidelné samokontroly, naše AI analýza kůže a včasné návštěvy u dermatologa jsou klíčové pro prevenci a včasné odhalení.
Navštiv dermatologa, pokud je hnědá skvrna nová, mění se, je velmi tmavá, nepravidelná nebo začíná svědit, krvácet nebo tvořit krusty, nebo pokud máš mnoho slunečních skvrn a historii intenzivního vystavení slunci. Rutinní kontroly každých 1-2 roky jsou rozumné, pokud je ti více než 35 let, máš světlou pleť nebo mnoho pigmentovaných lézí. Používej naši AI analýzu kůže mezi návštěvami, abys sledoval své skvrny a rozhodl, kdy něco potřebuje profesionální pohled.
Většina lentig není naléhavá a může být zkontrolována při plánované návštěvě dermatologa. Pokud se však skvrna, která vypadá jako sluneční nebo věková skvrna, začne rychle měnit, stane se velmi tmavou nebo nepravidelnou, nebo začne svědit, krvácet nebo tvořit krusty, měl bys navštívit dermatologa během několika týdnů, nikoli měsíců.