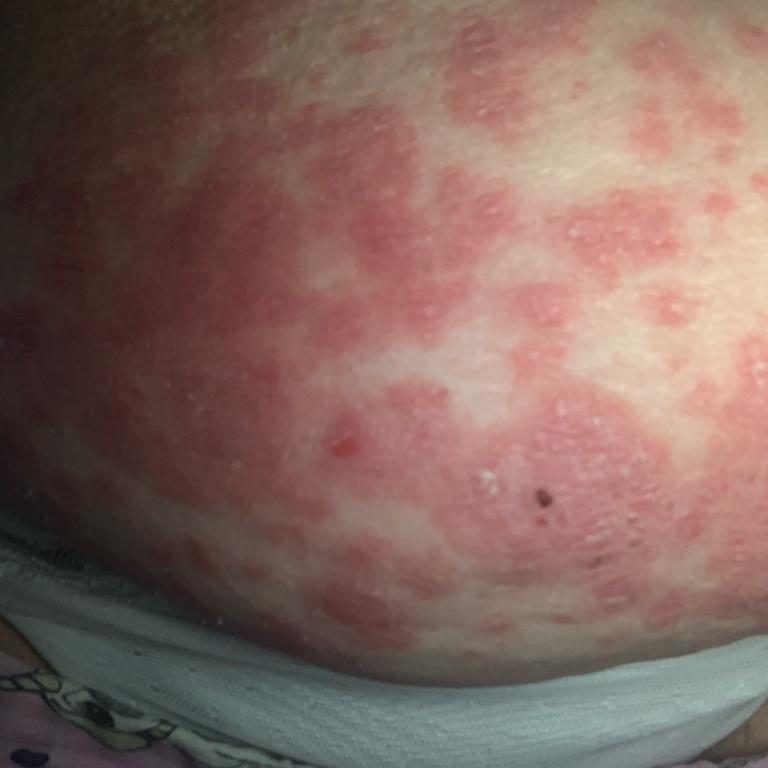
De exacte oorzaak van pustuleuze psoriasis is niet volledig begrepen, maar het omvat een overactieve immuunrespons bij genetisch gepredisponeerde mensen. Opflakkeringen worden vaak veroorzaakt door bepaalde medicijnen, plotselinge steroïdeonttrekking, infecties, roken, stress of sterke huidirritatie.
Je loopt een hoger risico op pustuleuze psoriasis als je al psoriasis hebt, rookt, bepaalde medicijnen gebruikt of plotselinge veranderingen in steroïdebehandeling hebt. Gegeneraliseerde vormen kunnen het hele lichaam aantasten en kunnen leiden tot ernstige complicaties die het bloed, de nieren en de lever betreffen.
De behandeling richt zich op het kalmeren van ontstekingen, het verwijderen van dikke schubben en het voorkomen van complicaties, met behulp van een mix van crèmes en systemische medicijnen. Afhankelijk van de ernst kunnen artsen keratolytische crèmes, topische steroïden, calcineurineremmers, retinoïden, immunosuppressiva en moderne biologische geneesmiddelen gebruiken, plus fototherapie in stabiele gevallen.
Je kunt pustuleuze psoriasis niet volledig voorkomen, maar je kunt opflakkeringen verminderen door niet te roken, alcohol te beperken, bekende medicijntriggers en agressieve huidirriterende stoffen te vermijden, en stress en gewicht onder controle te houden. Regelmatige controles en vroege aanpassing van de behandeling, ondersteund door onze AI-huidanalyse, helpen de ziekte stabieler te houden.
Wanneer een Dokter Te Zien?
Iedereen met vermoedelijke pustuleuze psoriasis moet een dermatoloog raadplegen, en gegeneraliseerde of snel verslechterende gevallen hebben vaak dringende ziekenhuiszorg nodig. Voortdurende follow-up is belangrijk om de huid te monitoren, systemische behandeling aan te passen en complicaties te screenen.
Gelokaliseerde, stabiele pustuleuze psoriasis moet binnen enkele weken door een dermatoloog worden beoordeeld, maar elke plotselinge opflakkering met wijdverspreide pustels, koorts of zich erg onwel voelen heeft dezelfde dag dringende of spoedeisende zorg nodig. Gegeneraliseerde pustuleuze psoriasis kan levensbedreigend zijn als het niet snel wordt behandeld.