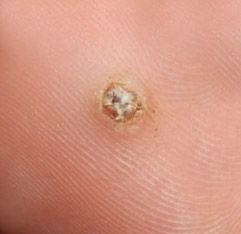
Підошовні бородавки викликані інфекцією шкіри вірусом папіломи людини (ВПЛ), зазвичай низькоризиковими типами, які не схильні викликати рак. Вірус проникає через крихітні тріщини в шкірі, особливо на вологих, пом'якшених підошвах, що піддаються впливу в таких місцях, як басейни, душі та спортзали. Не всі, хто піддається ВПЛ, отримують бородавки; слабкий імунітет, хронічні пошкодження шкіри, діабет, ожиріння та погана гігієна можуть збільшити ризик. Вагітність, стрес та серйозні інфекції також можуть знижувати ваші захисні сили та робити бородавки більш ймовірними.
Підошовні бородавки самі по собі вважаються доброякісними і мають дуже низький ризик перетворення на рак. Основні проблеми — це біль при ходьбі, кровотеча або інфекція, якщо їх зірвати або пошкодити, і поширення на інші ділянки або людей. Дуже швидке зростання, велика зміна кольору або форми, або новий сильний біль або свербіж повинні бути перевірені лікарем, щоб виключити інші пухлини шкіри. Множинні або рецидивуючі бородавки також можуть сигналізувати про ослаблену імунну систему або хронічне носійство ВПЛ.
Підошовні бородавки можна лікувати деструктивними методами, такими як лазер, кріотерапія рідким азотом, радіочастотне видалення або електрокоагуляція. Якщо є сумніви щодо діагнозу або якщо менш інвазивні методи неможливі, використовується хірургічне видалення з гістологією. Самостійне вирізання, спалювання або здирання бородавок вдома небезпечно через кровотечу, інфекцію, рубці та ризик пропустити рак шкіри. Навіть після успішного видалення бородавки можуть рецидивувати, тому важливі подальший догляд та профілактика.
Ви можете знизити ризик підошовних бородавок, захищаючи ноги в громадських душах, басейнах і спортзалах, і не ходячи босоніж у цих місцях. Тримайте ноги чистими і сухими, змінюйте шкарпетки щодня і носіть добре підібране взуття, щоб уникнути хронічного тертя і невеликих пошкоджень шкіри. Підтримуйте свою імунну систему хорошим сном, харчуванням і своєчасним лікуванням інфекцій і хронічних захворювань, таких як діабет. Після появи або видалення бородавки обмежте вплив УФ на цю ділянку, уникайте повторних травм і регулярно перевіряйте шкіру або використовуйте наш AI-аналіз шкіри для моніторингу.
Коли звернутися до лікаря?
Більшість підошовних бородавок не є терміновими, але вам слід звернутися до дерматолога, якщо вони болючі, поширюються, кровоточать або не покращуються при простому догляді. Вам також слід перевіритися, якщо ураження виглядає незвично для бородавки, швидко змінюється, або якщо у вас діабет, поганий кровообіг або слабка імунна система. Наш AI-аналіз шкіри може допомогти вам відстежувати бородавку між візитами, але не замінює особистий огляд і біопсію, коли це необхідно.
Підошовні бородавки зазвичай є проблемою низької терміновості і можуть бути оцінені дерматологом на рутинній основі, особливо якщо вони стабільні і лише злегка незручні. Зверніться за ранньою допомогою, якщо ураження швидко змінюється, стає дуже болючим, кровоточить, виглядає нетипово для бородавки, або якщо у вас діабет, поганий кровообіг або слабка імунна система.