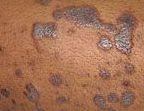
De exacte oorzaak van lichen planus is onbekend, maar men denkt dat het gerelateerd is aan een overactieve immuunrespons. Bij sommige mensen kan het worden veroorzaakt door bepaalde medicijnen, hepatitis C-infectie of contact met giftige stoffen zoals zware metalen.
Lichen planus komt vaker voor bij volwassenen, vooral bij mensen van middelbare leeftijd, en iets vaker bij vrouwen. De risico's zijn hoger als je bepaalde auto-immuunziekten hebt, chronische hepatitis C, of medicijnen gebruikt die bekend staan om vergelijkbare uitslag te veroorzaken.
Lichen planus verbetert vaak vanzelf, maar behandeling kan jeuk, pijn verlichten en complicaties zoals littekens of haarverlies voorkomen. Veelgebruikte behandelingen zijn onder meer topische steroïde crèmes, antihistaminica voor jeuk, UV-lichttherapie en in hardnekkige gevallen medicijnen zoals retinoïden of tacrolimus.
Er is geen gegarandeerde manier om lichen planus te voorkomen, maar je kunt opflakkeringen verminderen door huidletsel te vermijden, stress te beheersen en medicijnen te herzien die vergelijkbare uitslag kunnen veroorzaken. Voor mondbetrokkenheid zijn niet roken, het vermijden van alcohol en zachte mondverzorging essentieel.
Wanneer een Dokter Te Zien?
Je moet een dermatoloog raadplegen om de diagnose te bevestigen, op lijkende aandoeningen uit te sluiten en behandeling te krijgen als je sterke jeuk, zweren in de mond of geslachtsdelen, nagelveranderingen of haarverlies op de hoofdhuid hebt. Regelmatige follow-up is belangrijk voor langdurige orale of genitale lichen planus.
Lichen planus is meestal geen noodgeval, maar je moet binnen een paar weken een routinematige dermatologische afspraak maken, eerder als je pijnlijke zweren in de mond of geslachtsdelen, nagelvernietiging of tekenen van haarverlies op de hoofdhuid hebt.