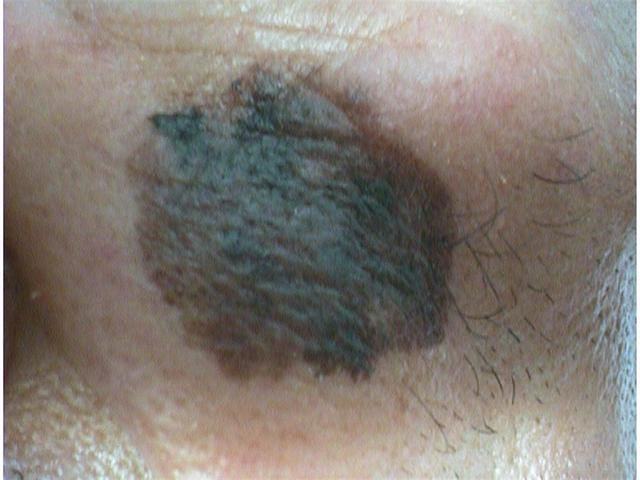
เลนติโก เมลาโนมา เกิดจากความเสียหายจากแสงแดดสะสมในระยะยาวต่อผิวหนัง โดยเฉพาะบนใบหน้า นำไปสู่การเปลี่ยนแปลงของเซลล์เม็ดสีในแผ่นที่มีอยู่ก่อนเรียกว่า เลนติโก มาลิกนา พันธุกรรม ผิวขาว และภูมิคุ้มกันต่อต้านเนื้องอกที่ลดลงก็มีบทบาทในผู้ที่พัฒนาเมลาโนมาชนิดนี้
เลนติโก เมลาโนมา มีความเสี่ยงสูงต่อการกลับมาในท้องถิ่นและการแพร่กระจายไปยังต่อมน้ำเหลืองและอวัยวะภายในเมื่อมันบุกรุกชั้นผิวหนังที่ลึกขึ้น ความเสี่ยงสูงกว่าในผู้สูงอายุที่มีผิวขาวที่มีการสัมผัสแสงแดดตลอดชีวิตอย่างหนัก ประวัติการถูกแดดเผา หรือเมลาโนมาก่อนหน้านี้
การรักษาหลักสำหรับเลนติโก เมลาโนมา คือการผ่าตัดเอาออกกว้าง ๆ ด้วยขอบความปลอดภัย บางครั้งรวมกับการผ่าตัดต่อมน้ำเหลืองหากสงสัยว่ามีการแพร่กระจาย ในกรณีที่มีความก้าวหน้ามากขึ้น การรักษาเพิ่มเติมเช่นการบำบัดด้วยภูมิคุ้มกัน การบำบัดแบบมุ่งเป้า เคมีบำบัด หรือการฉายรังสีอาจถูกใช้ ในขณะที่วิธีการทำลายท้องถิ่นเช่นเลเซอร์หรือการแช่แข็งไม่เหมาะสมสำหรับมะเร็งชนิดนี้