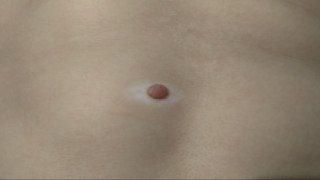
Точната причина за хало невус не е напълно разбрана, но е свързана с имунната система, която атакува пигментните клетки в и около бенката. Генетика, витилиго, автоимунни състояния и UV излагане могат да играят роля. Резултатът е загуба на пигмент около бенката, образувайки белия хало.
Сам по себе си, хало невус се счита за безопасен и не увеличава значително риска от меланом. Основната загриженост е, когато бенка в хало изглежда нетипична или започва бързо да се променя. Всяка бърза промяна, нови симптоми или много неправилни характеристики трябва да бъдат проверени от дерматолог.
Повечето хало невуси не изискват никакво лечение и могат просто да бъдат наблюдавани с времето. Ако бенка изглежда подозрителна, е многократно травмирана или се променя по тревожен начин, се препоръчва хирургично отстраняване с хистология. Разрушителни методи като лазер или замразяване не са идеални, защото унищожават тъканта, необходима за правилно изследване.
Не можеш напълно да предотвратиш хало невусите, защото те са задвижвани от имунната ти система и генетиката, но можеш да защитиш кожата си като цяло. Ограничете UV излагането, избягвайте солариумите и използвайте слънцезащитен крем и дрехи, за да намалите увреждането от слънцето. Опитайте се да избягвате хронично триене или нараняване на бенки и следете за всякакви промени.
Посети дерматолог, ако хало невус изглежда много различен от другите ти бенки, променя се бързо или започва да сърби, боли, кърви или образува корички. Рутинни проверки на всеки 1-2 години са добра идея, ако имаш много бенки, история на рак на кожата или множество хало невуси.
Типичен, стабилен хало невус не е спешен случай и може да бъде проверен при рутинно посещение при дерматолог. Ако бенката в хало се променя бързо, изглежда много неправилна или започва да сърби, боли или кърви, трябва да уредиш не-спешен, но бърз преглед в рамките на няколко седмици.