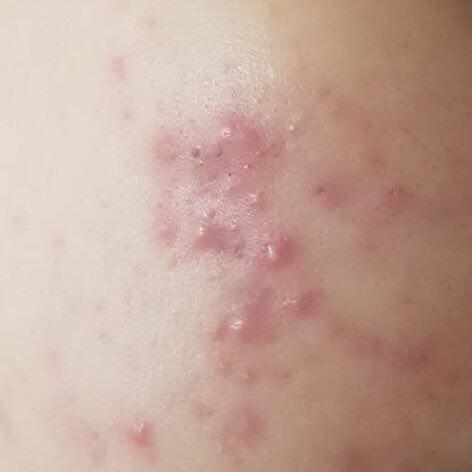
Forbraíonn acne pustular nuair a spreagann sebum iomarcach, pores clogged agus baictéir craicinn athlasadh sna follicles gruaige, ar chúlra tionchair ghéiniteacha agus hormónacha. Is féidir le caithreachas, androgens, strus, cosmaidí, frithchuimilt, agus aiste bia go léir cur leis, ach is annamh a bhíonn cúis aonair leithlisithe.
De ghnáth ní bhíonn acne pustular contúirteach, ach is féidir leis scars buana, spotaí dorcha agus strus síceolaíoch suntasach a chur faoi deara mura ndéantar é a chóireáil i gceart. I gcásanna annamh, is féidir le acne dian nó neamhaird a bheith ionfhabhtaithe go mór nó fadhbanna hormónacha nó meitibileacha bunúsacha a léiriú.
De ghnáth bíonn cóireáil acne pustular ag comhcheangal táirgí frith-athlastacha agus frith-baictéarach tráthúla, retinoids chun casadh craicinn a normalú, agus cúram cosmaideach éadrom. I gcásanna níos déine nó níos frithsheasmhaí, féadfaidh dochtúirí antaibheathaigh ó bhéal, teiripe hormónach nó nósanna imeachta cosúil le teiripe solais, peels nó léasair a chur leis chun athlasadh a laghdú agus scars a fheabhsú.
Is féidir leat cabhrú le lasracha acne pustular a chosc trí chúram craicinn neamh-comedogenic éadrom a úsáid, piocadh a sheachaint, do chraiceann a chosaint ó sholas iomarcach agus frithchuimilt, agus stíl mhaireachtála agus aiste bia sláintiúil a choinneáil. Laghdaíonn seiceálacha féin rialta agus coigeartú luath cúraim le deirmeolaí nó anailís AI ar an gcraiceann an baol scars agus spotaí dorcha.
Cathain le Feiceáil do Dhochtúir?
Féach le deirmeolaí le haghaidh acne pustular mura bhfuil táirgí thar an gcuntar ag cabhrú tar éis cúpla seachtain, má fheiceann tú nodules, cysts nó scars, nó má tá tionchar láidir ag acne ar do ghiúmar nó do fhéinmheas. Cabhraíonn leanúint rialta agus úsáid ár n-anailís AI ar an gcraiceann idir chuairteanna le cóireáil a mhionchoigeartú agus damáiste fadtéarmach a chosc.
De ghnáth ní éigeandáil é acne pustular, ach ba chóir duit deirmeolaí a fheiceáil laistigh de chúpla seachtain chun scars agus spotaí dorcha a chosc, go háirithe má tá sé forleathan nó ag cur isteach ort go mothúchánach. Lorgaigh cúram níos práinní má tá léasanna an-phianmhar, ag dul in olcas go tapa, nó ag gabháil le fiabhras nó ag mothú míshláintiúil.